New Pain-Free Alternative to Biopsy: evaluation, treatment and follow-up options for Hepatitis C patients


Assessing liver fibrosis in Hepatitis C patients used to lead to a “least worst” decision: would it be better to treat the patient with early generation antiviral therapies, exposing him or her to damaging side effects for a 50/50 shot at a cure, or should the patient be monitored, via regular liver biopsies, as the untreated disease progresses?
New oral drugs have changed this calculus for Hepatologists. These drugs cure the disease in more than 90 percent of patients, have fewer side effects, and can work much faster than earlier treatment options. Since the new therapies are so effective, precise staging is no longer required as a means to triage patients to treatment. Hepatologists no longer have to subject patients to painful liver biopsies to gain the staging information necessary for treatment decisions. The most important determination is the identification of cirrhosis so that appropriate long-term follow-up can be initiated following curative therapy. These developments in treatment dovetail with developments in liver evaluation technology. Instead, using ShearWave™ Elastography (SWE), they can perform a non-invasive test in the office and obtain results about tissue stiffness and the extent of liver fibrosis in real time.
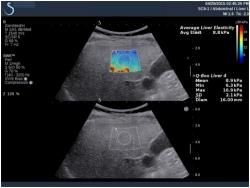
Fig. 1. After treatment, a patient demonstrates a F2/F3 Fibrosis of the Liver with SWE.
ShearWave™ Elastography (SWE)
ShearWave is a form of ultrasound elastography that uses fast-moving shear waves to determine tissue stiffness, which is an important diagnostic tool for staging chronic liver disease. To achieve real-time quantification of tissue stiffness demands a high-speed acquisition of images. The SWE color-coded map provides the ability to visualize and analyze tissue stiffness during an examination.
Avoiding Invasive Procedures
According to an American Association for the Study of Liver Diseases position paper, in 2009 the three major roles of liver biopsy were: 1) diagnosis, (2) disease staging, and/or (3) assistance for making therapeutic management decisions. The authors noted, however, that non-invasive alternatives “may replace use of liver histology in [prognosis and treatment], particularly with regard to assessment of the severity of liver fibrosis.” The advances in Hepatitis C treatment since then make that prediction accurate.
Biopsies pose relatively small risks of morbidity and an extremely small risk of mortality, but their more common risks are still a burden for patients: between 25% and 30% experience pain, for instance, and the duration of the procedure plus a recovery period is several hours. Possible complications include bleeding that requires hospitalization or transfusion or the puncture of a surrounding organ. In addition to those burdens, a liver biopsy costs between $1,500 and $2,000 when there are no complications.
The risks of an invasive procedure might outweigh the benefits of a non-invasive alternative, of course, if the results were more accurate or better suited to the available treatment options. But in the case of liver fibrosis, a SWE scan can sometimes overcome biopsy’s sampling limitations. SWE can reduce the possibility of sampling error that arises from the very nature of a biopsy –that is, the selective sampling of a large organ. Using ultrasound-guided imaging technology to zero in on areas of interest in real time can thus prevent the need for follow-ups due to variability in sampling. This is not a small consideration, as eliminating a follow-up biopsy can decrease the patient’s time in the clinic, likely increasing their satisfaction, and improving clinical throughput.
Improving Follow-Up Experience
With the most recent oral medications, about 90 percent of Hepatitis C patients are cured of the virus. Those patients still need to be evaluated after taking the drug to assess their progress. SWE is also useful for such required follow-up appointments, as those benefits are easy to discern with the technique. Perhaps more importantly from a patient perspective, SWE can show the patient his or her progress: the physician can call up an earlier scan of the same region and compare it to the real-time scan to chart the change.
With SWE, a post-treatment follow-up takes up two minutes of a regular clinic visit, and takes biopsies largely out of the equation. Instead of a series of follow-up biopsies, a patient will need to come in only once a year for a quick SWE check-up.
Conclusion
SWE is a promising pain-free option for Hepatitis C patients but, as with any new technologies, there may be clinical situations where the technique is less effective. Clinicians have been pleased with results to date, and will continue to learn more as it becomes standard practice and through additional research as it becomes available. Patients are now able to look forward to pain free evaluations and follow-up appointments with their physician, as they progress through the phases of treatment given the advances in technology now available
[1] http://www.niaid.nih.gov/news/newsreleases/2015/Pages/HepatitisCTripleDrug.aspx
[2] http://www.aasld.org/sites/default/files/guideline_documents/LiverBiopsy2009.pdf
[3] http://www.aasld.org/sites/default/files/guideline_documents/LiverBiopsy2009.pdf
[4] http://hcvadvocate.org/hepatitis/factsheets_pdf/Biopsy.pdf






1 Comment
Great News……….. (Y)