Gastroenterology: Ascites
University of Iowa Family Practice Handbook, 3rd Edition, Chapter 4
Peter P. Toth, M.D., Ph.D.
Department of Family Medicine
University of Iowa
Peer Review Status: Externally Peer Reviewed by Mosby
- Ascites is a pathologic accumulation of serous fluid within the abdomen. It may be caused by decompensated liver disease (alcohol- and virus-related cirrhosis), heart failure, abdominal carcinomatosis, tuberculosis, and pancreatic disease. Cirrhosis is the cause for the most number of cases of ascites.
- Diagnostic paracentesis can confirm the diagnosis of portal hypertension or rule out the possibility of infection. The following tests should be performed on ascites fluid: cell count, cytology, culture (in blood culture bottles), Gram stain, total protein, glucose, lactate dehydrogenase, amylase, and, if warranted, mycobacterial smear and culture. Samples with
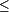 250 neutrophils per milliliter are assumed to be infected, and broad-spectrum antibiotic therapy should be initiated. Patients with a total protein concentration
250 neutrophils per milliliter are assumed to be infected, and broad-spectrum antibiotic therapy should be initiated. Patients with a total protein concentration 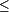 1.0 g/dl are at high risk for spontaneous bacterial peritonitis. There is good evidence that Bactrim (1 DS tablet daily 5 days a week) is effective in preventing spontaneous bacterial peritonitis and decreasing mortality. Norfloxacin has been used as well, but its use is discouraged because of the rapid development of resistant organisms.
1.0 g/dl are at high risk for spontaneous bacterial peritonitis. There is good evidence that Bactrim (1 DS tablet daily 5 days a week) is effective in preventing spontaneous bacterial peritonitis and decreasing mortality. Norfloxacin has been used as well, but its use is discouraged because of the rapid development of resistant organisms. - Therapeutic paracentesis with the removal of 5 or moreLiters is indicated if the patient presents with early satiety or shortness of breath. After the procedure, give 40 g of albumin IV to prevent hyponatremia and renal failure.
- The serum-ascites albumin gradient is equal to [albumin]serum – [albumin]ascites. If the gradient exceeds 1.1 g/dl, the patient has portal hypertension.
- Treatment consists in restricting sodium intake and the promotion of natriuresis with oral diuretics. Combinations of furosemide and spironolactone have been shown to be optimal for promoting sodium excretion and sparing potassium. Doses should be titrated to a maximum of 400 mg/day and 160 mg/day of spironolactone and furosemide respectively. Serial determinations of urinary sodium excretion may help to guide dosing. Other therapies include portal shunting and liver transplantation. Overaggressive diuresis is associated with hepatorenal syndrome (a relatively acute, progressive renal failure in the patient with advanced liver disease secondary to decreased renal perfusion) and is discouraged. Large-volume paracentesis is preferable.




