Subclinical Hepatic Encephalopathy Impairs Daily Functioning
HEPATOLOGY, July 1998, p. 45-49, Vol. 28, No. 1
Original Articles
Michael Groeneweg1, Juan C. Quero1, Ilone De Bruijn1, Ieneke J. C. Hartmann1, Marie-louise Essink-bot2, Wim C. J. Hop3, and Solko W. Schalm1
From the Departments of 1 Hepatogastroenterology, 2 Public Health, and 3 Biostatistics, Erasmus University Hospital, Dr. Molewaterplein 40, 3015 GD Rotterdam, the Netherlands.
ABSTRACT
Subclinical hepatic encephalopathy (SHE) is assumed to have a negative effect on patients’ daily functioning; therefore, treatment is recommended. However, no studies have been performed that document the clinical relevance of SHE. We performed a study in which the prevalence of SHE was determined in 179 outpatients with cirrhosis using two psychometric tests (Number Connection Test Part A [NCT-A] and the Digit Symbol Test [DGT]) and automated analysis of the electroencephalogram (EEG). SHE was defined by the presence of at least one abnormal psychometric test and/or abnormal slowing of the EEG. The influence of cirrhosis and SHE on patients’ daily functioning was assessed using the Sickness Impact Profile (SIP) questionnaire. The distribution of SIP scores of the patients with cirrhosis differed from the reference scores of the general population. Patients with cirrhosis and SHE (n = 48) reported significantly more impairment in all 12 scales of the SIP, in the psychosocial subscore, the physical subscore, as well as in the total SIP score, compared with cirrhotic patients without SHE (n = 131). Multivariate analysis taking into account severity of liver disease (Child-Pugh score), presence of varices, and alcoholic etiology, showed that SHE independently was related to a diminished total SIP score. The reproducibility of the SIP was high when the test was repeated after a 3-month period. We conclude that SHE implies impaired daily functioning and warrants attempts at treatment. (HEPATOLOGY 1998;28:45-49.)
INTRODUCTION
Clinical manifestations of hepatic encephalopathy include a decreased intellectual function, personality disorders, an altered level of consciousness, and neuromuscular dysfunction.1 In addition to clinical manifest hepatic encephalopathy,2 a subclinical stage has been described, which cannot be detected through global clinical examination, but requires specific neuropsychological and neurophysiological examination.3-12 The prevalence of subclinical hepatic encephalopathy (SHE) is estimated to vary from 30% to 84% according to recent studies using appropriate methods.12-16 This variation in reported prevalence depends on the kind (psychometric or electrophysiological) and number of tests used, and the population (etiology and severity of the liver disease) tested.17
SHE is considered to be clinically relevant for two reasons. First, it could be a preceding stage of clinical manifest hepatic encephalopathy.3 However, this assumption is not proven, because only one follow-up study16 supports this concept. Second, the psychomotor deficits found in SHE could have a disadvanting influence on patients’ daily functioning, e.g., driving a car or performing at work.18 In view of the reported high prevalence of SHE and its presumed negative effect on daily life, routine screening of cirrhotic patients for SHE and treatment of SHE is recommended.19-21 However, the need of treatment of SHE is questionable, because a recent study has shown that patients with SHE did not perform worse driving “on the road” than patients without SHE.22 Driving a car is an important, but small, part of the total spectrum of daily activities. Therefore, on the basis of this study, no conclusions can be made about the effect of SHE on other aspects of daily functioning.
The influence of chronic diseases on daily life can be assessed using “Health-related Quality of Life” questionnaires.23 The “Sickness Impact Profile” (SIP) questionnaire24,25 is such an instrument for overall health assessment and has been used before to determine the influence of chronic liver disease on patients’ daily functioning.26-29
The aim of the present study was to determine the prevalence of neuropsychological and neurophysiological defects in stable cirrhotic patients attending a university hospital outpatient clinic using two neuropsychological tests and the neurophysiological method of automated analysis of the electroencephalogram (EEG). The SIP questionnaire was used to determine the influence of SHE on daily functioning. In addition, the reproducibility of the SIP in cirrhotic patients was determined.
PATIENTS AND METHODS
Subjects and Investigations
From January 1, 1992, to May 1, 1996, 202 consecutive patients attending the outpatient clinic of Hepatogastroenterology of the University Hospital Rotterdam were screened for SHE. Inclusion criteria were: histologically proven cirrhosis and age between 16 and 80 years. One hundred ninety-three of 202 patients fitted the inclusion criteria; 3 patients had a surgically constructed portacaval shunt (no cirrhosis), and 6 patients only had clinical signs of cirrhosis at screening. Exclusion criteria were: clinical manifest hepatic encephalopathy*; history of recent (less than 6 weeks) alcohol abuse; use of benzodiazepines, anti-epileptics, or other psychotropic drugs; inability to perform the psychometric tests and to complete the SIP questionnaire (caused by either insufficient knowledge of the Dutch language or bad vision); and severe medical problems such as congestive heart failure, pulmonary disease, neurological disease, etc., that influence the quality-of-life measurement.
In the final analysis, a total of 179 patients with histologically proven cirrhosis were included. Fourteen patients were excluded because of incomplete SHE screening and/or inability to fill out the quality-of-life questionnaire.
All patients underwent a clinical and laboratory investigation, psychometric tests, and automated EEG analysis. In addition, the SIP questionnaire was administered. All examinations took place on the same day. Test-retest reliability of the SIP was assessed by re-administering the questionnaire to patients without signs of decompensated liver disease (i.e., jaundice, ascites, encephalopathy, or variceal bleeding) after a 3-month period.
Clinical and Laboratory Assessment
The Child-Pugh score was used to assess the severity of liver disease.31 Three biochemical variables (serum albumin, bilirubin, and prothrombin time) in addition to the two clinical characteristics (presence or absence of ascites and clinical signs of encephalopathy) determine the Child-Pugh score. Each variable is given 1 to 3 points, leading to scores ranging from 5 (excellent liver function) to 15 points (poor liver function).
Presence of esophageal or gastric varices was evaluated, using reports of endoscopic investigations in 174 patients, and esophageal x-rays in 5 patients.
Alcoholic etiology of cirrhosis was defined as: presence of severe alcohol abuse in patient history and absence of other etiological factors.
Neuropsychological Assessment
Number Connection Test Part A. This test is a derivative from the Trail Making Test32 and measures cognitive motor abilities. In the Number Connection Test Part A (NCT-A), patients must connect numbers printed on paper consecutively from 1 to 25. Age-related normal values of this NCT-A have been developed in 681 persons without liver disease.33 Normal values are expressed as the mean ± 2 SD. After explanation, abbreviated demonstration tests were administered to be sure the patient had understood it. Errors were not enumerated, but patients were instructed to return to the preceding correct number and then carry on. The test score is the time the patient needs to perform the test, including the time needed to correct the errors. A low score indicates a good performance.
Digit Symbol Test. This is a subtest of the Wechsler Adult Intelligence Scale and measures motor speed and accuracy.34 The patient is given a list of digits from 1 to 9 associated with symbols and is asked to fill in blanks with symbols that correspond to each number. The test score is the total number of correct sequential matchings of symbols to numbers in a 90-second interval. The normative data used are expressed as percentiles. After explanation of each test, an abbreviated demonstration was administered to ensure that the patient understood the test correctly. A high score indicates a good performance. Data of 2,169 Dutch and Belgian healthy controls served as a reference group in the Netherlands.35 A test result below the 2.5th percentile (i.e., the mean -2 SD) is considered abnormal.
Neurophysiological Assessment
The EEG was recorded using standardized techniques while the patient, with the eyes closed, laid comfortably in a quiet room. When drowsiness occurred, an auditory stimulus was applied by the EEG technician. Five electrodes were attached to the skin at the positions T3, T4, O1, O2, and Cz according to the international “10-20 system.”36 Electrode impedance was kept lower than 5 k![]() . After applying the usual band-pass filters (0.53-35 Hz), two runs of 100 seconds each were recorded and compared for reproducibility. Artefact-free recordings were selected and fed into a computer after analogue-digital conversion (sample frequency, 102.4 Hz). Ten epochs of 10 seconds each were analyzed by applying Fast Fourier Transformation and the mean power spectrum calculated. Patients are graded in the different stages of hepatic encephalopathy on account of their mean dominant frequency, and the relative powers of delta and theta activity. In a previous study,37 we have validated this method in 51 healthy controls (median age, 41 years; range, 21-78 years) and 66 patients with cirrhosis (median age, 60 years; range, 21-75 years). A theta activity above 35% (i.e., the mean + 2 SD in controls) is considered abnormal.
. After applying the usual band-pass filters (0.53-35 Hz), two runs of 100 seconds each were recorded and compared for reproducibility. Artefact-free recordings were selected and fed into a computer after analogue-digital conversion (sample frequency, 102.4 Hz). Ten epochs of 10 seconds each were analyzed by applying Fast Fourier Transformation and the mean power spectrum calculated. Patients are graded in the different stages of hepatic encephalopathy on account of their mean dominant frequency, and the relative powers of delta and theta activity. In a previous study,37 we have validated this method in 51 healthy controls (median age, 41 years; range, 21-78 years) and 66 patients with cirrhosis (median age, 60 years; range, 21-75 years). A theta activity above 35% (i.e., the mean + 2 SD in controls) is considered abnormal.
Assessment of Daily Functioning
The SIP questionnaire is an often-used instrument that assesses the influence of disease and treatment on daily functioning.24 The questionnaire consists of 136 items, which are grouped into 12 scales: sleep and rest, eating, work, home management, recreation and pastimes, ambulation, mobility, body care and movement (scores of the latter three may be combined as a physical subscore), social interaction, alertness behavior, emotional behavior, and communication (scores of the latter four may be combined as a psychosocial subscore). Apart from a 12-dimensional profile score and the physical and psychosocial scores, the SIP provides the opportunity to compute a total score. Each score ranges from 0 (best score) to 100 (worst score). Patients mark only items that relate to their health at that time. The SIP has been translated and validated for the Dutch population.38,39
Statistical Analysis
Fisher’s Exact test was used to assess differences in sex (male:female), age-group (<60 years: ![]() 60 years), Child-Pugh score (A:B/C), etiology of cirrhosis (alcohol:other), and presence of varices between patients with and without SHE. Difference in median age was tested, using the Wilcoxon rank sum test. Those variables reaching (borderline) statistical significance in the univariate analysis were selected for multivariate analysis, using multiple regression to determine their influence on total SIP score. In this analysis, total SIP scores were logarithmically transformed to reduce skewness of distributions. The limit for statistical significance was set at P = .05. Test-retest reliability (reproducibility) was assessed using intraclass correlation coefficients. Values above 0.7 generally are considered to indicate good reliability.40 Internal consistency reliability of the SIP scales was assessed using Cronbach’s .41 The internal consistency of a multi-item scale is a measure of the homogeneity of the items. An of 0.70 is considered to demonstrate good internal consistency.42
60 years), Child-Pugh score (A:B/C), etiology of cirrhosis (alcohol:other), and presence of varices between patients with and without SHE. Difference in median age was tested, using the Wilcoxon rank sum test. Those variables reaching (borderline) statistical significance in the univariate analysis were selected for multivariate analysis, using multiple regression to determine their influence on total SIP score. In this analysis, total SIP scores were logarithmically transformed to reduce skewness of distributions. The limit for statistical significance was set at P = .05. Test-retest reliability (reproducibility) was assessed using intraclass correlation coefficients. Values above 0.7 generally are considered to indicate good reliability.40 Internal consistency reliability of the SIP scales was assessed using Cronbach’s .41 The internal consistency of a multi-item scale is a measure of the homogeneity of the items. An of 0.70 is considered to demonstrate good internal consistency.42
RESULTS
One hundred seventy-nine patients with histologically proven cirrhosis (113 male, 66 female; mean age, 50 years; SD 14; range, 18-77 years) entered the final analysis. The etiology of cirrhosis was chronic viral hepatitis in 71 patients, alcohol abuse in 38 patients, and other causes (e.g., autoimmune, primary biliary cirrhosis, cryptogenic) in 70 patients. None of the patients had evidence of neurological and/or psychiatric abnormalities on global clinical examination performed in each patient by one of the first two authors (M.G. and J.C.Q.).
table 1 summarizes the prevalence of abnormality in age-related psychometric tests and automated EEG analysis found in the study population. Forty-eight patients had slowing of the EEG (at least grade 1 by spectral analysis) and/or at least one abnormal psychometric test. These 48 patients were considered as having SHE, while the remaining 131 patients were considered not to have SHE.15 Clinical and laboratory characteristics of both patient groups are summarized in table 2. The male/female ratio did not differ between groups. Patients with SHE had a more severe liver disease, as quantified by the Child-Pugh score, and more often had esophageal or gastric varices. Moreover, patients with SHE more often had alcoholic etiology of cirrhosis and they tended to be older: 55 (36-74) years versus 50 (18-77) (median age [range]) years for cirrhotic patients without SHE. However, no difference was found in the number of patients older than 60 years of age (table 2).
| table 1. Prevalence of Abnormal Neuropsychological and Neurophysiological Tests and the Diagnosis of SHE in 179 Cirrhotic Patients Without Clinical Signs of Hepatic Encephalopathy |
| table 2. Clinical and Laboratory Characteristics of Cirrhotic Patients With and Without SHE |
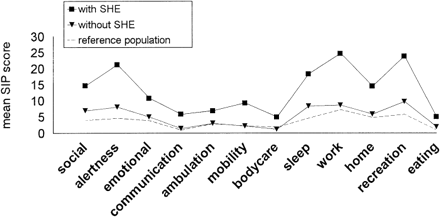
Figure 1 shows that the mean SIP scores of patients with and without SHE compared with reference scores of the general population.39 Patients with cirrhosis and SHE reported significantly more impairment in all 12 scales of the SIP, in the psychosocial subscore, the physical subscore, as well as in the total SIP score, compared with cirrhotic patients without SHE (table 3).
| Fig. 1. Mean SIP scale scores in 131 cirrhotic patients without SHE and 48 cirrhotic patients with SHE, compared with a reference group of 594 Dutch persons (Jacobs39).
|
| View This table | table 3. SIP Scores of Cirrhotic Patients With and Without SHE |
Separate analysis of total SIP score in patients with abnormal psychometric tests, or with an abnormal EEG or with both abnormal psychometric test(s) and abnormal EEG, showed equally impaired total SIP scores: for psychometric tests: 14 (0.4-18.6); for EEG: 11.2 (8.4-14); and for both psychometric tests and EEG: 13.5 (6.9-20.2) versus 4.6 (3.7-5.5) (mean [95% confidence interval of mean] for cirrhotic patients with normal test results [no SHE]).
The results of the SIP scores were similar between the various etiologies of chronic liver disease. Although patients with SHE more often had cirrhosis of alcoholic etiology, patients with alcoholic cirrhosis did not report more impairments on the psychosocial, physical, or on the total SIP score, compared with patients with nonalcoholic cirrhosis (data not shown).
Possible confounders in the analysis comparing patients with and without SHE could be the severity of liver disease (Child-Pugh score, presence of varices) and the etiology of cirrhosis (including fatigue as often observed in viral disease and primary biliary cirrhosis). Therefore, these variables were selected for multivariate analysis to evaluate their impact on total SIP score. This analysis showed that only presence of SHE and neither the Child-Pugh score, presence of varices, nor the etiology of cirrhosis significantly affects total SIP score (table 4).
| table 4. Effect of Presence of SHE, Child-Pugh Score, Etiology (alcohol vs. non-alcohol), and Presence of Varices on Total SIP Score |
Reliability testing of the SIP questionnaire in our patient population using internal consistency measures showed that 10 subscales of the SIP fell below the recommended coefficient of 0.70 (table 3). This finding suggests that the items of these SIP scales are not homogeneous in the population of patients with cirrhosis, i.e., the items of such a scale do not reliably represent an underlying characteristic.43 The high internal consistency of the total SIP score is at least partly attributable to the high number of items. The reproducibility of the SIP questionnaire was high, because we found a good correlation between the SIP results in a 3-month interval (table 5). Minor, statistically not significant, differences of mean SIP scores were found between the first and second completed SIP questionnaire, indicating that, during the 3 months, patients had not systematically changed with regard to the SIP questionnaire.
| table 5. SIP Scores of 38 Cirrhotic Patients at Baseline and After 3 Months |
DISCUSSION
We performed a study to determine the influence of SHE on the quality of life. Two psychometric tests with age-related normal values (NCT-A and DST) and automated EEG analysis were selected to be used as neuropsychological and neurophysiological screening tests for SHE.15 We defined SHE as presence of at least one abnormal psychometric test and/or abnormal slowing of the EEG (at least grade 1 by spectral analysis). Using this definition, we found a SHE prevalence of 27% in our outpatient cirrhotic population, which is in agreement with the prevalence found in studies using the same methods.13-15,17 We used the SIP as a method for evaluating the influence of SHE on daily functioning in cirrhotic patients, because this questionnaire contains items that resemble the complaints seen in early stages of hepatic encephalopathy. In addition, this questionnaire has been used in a previous study in patients with SHE.10
In our study, we found a diminished level of functioning in patients with SHE, as reflected by significantly more impairments in all 12 categories of the SIP. Highest scores were found on the categories of social interactions, alertness, emotional behavior, mobility, sleep/rest, home management, and recreation and pastimes. These are all items that are expected to be affected in cognitive disorders. Although the severity and etiology of liver disease could have influenced the total SIP scores, multivariate analysis showed that only the presence of SHE independently accounts for the total SIP score result.
Patients with hepatic encephalopathy grade 1 can complain about, for example, sleep disturbances, impaired calculation, shortened attention, mild personality changes, and muscular incoordination.44 Patients with SHE (in literature, considered as a preclinical stage of hepatic encephalopathy) should therefore, although to a lesser extent, have similar complaints in daily life. Our findings support this assumption.
How reliable are our findings? First, our study was performed in a large sample size (n = 179), which makes the results of the SIP more adequate for statistical analysis.
Second, SHE was diagnosed using a combination of neuropsychological and neurophysiological tests. We only used validated psychometric tests with age-related normal values, thereby abolishing the diagnostic bias caused by aging on neuropsychological performance.15,17 The fact that patients with abnormal psychometric tests as well as patients with an abnormal EEG showed more impairments in daily life supports the use of both neuropsychological and neurophysiological methods for the diagnosis of SHE.
Third, we used a validated test to evaluate daily functioning, with reference values for the Dutch population. In addition, we found a good test-retest reliability of the SIP in our patient population with cirrhosis.
Fourth, we tried to exclude confounding variables by applying multivariate analysis. Age, etiology, and severity of cirrhosis did not explain the difference in quality of life in cirrhotic patients with and without SHE; this finding also excludes that symptoms such as fatigue (a common symptom in viral disease and in primary biliary cirrhosis), explain the observed difference.
Lastly, our findings are logical.
Should we treat patients with SHE because of the diminished level of daily functioning found in this study? Up to now, no intervention studies have been performed, in which functional status is used as an outcome of treatment efficacy in SHE. Treatment of SHE could be beneficial in patients with stable liver disease and impaired performance at work or daily life. We therefore strongly suggest the use of “health-related quality-of-life questionnaires” in trials with treatment specifically directed to SHE. Footnotes
Abbreviations: SHE, subclinical hepatic encephalopathy; SIP, Sickness Impact Profile; EEG, electroencephalogram; NCT-A, Number Connection Test Part A; DST, Digit Symbol Test.
* Clinical manifest hepatic encephalopathy was assumed to be present if at least two of the following abnormalities were detected, or one abnormality in association with a flapping tremor30: inverted sleep pattern, impaired calculation, disturbed secondary memory, and slowness of speech. Impaired calculation was assessed by asking the patient to subtract serial sevens from 100 and to repeat a series of six nonconsecutive numbers in the same order (a normal individual can easily remember seven numbers forward). Memory was tested by asking the patient to remember three objects and to repeat these several minutes later, and by asking the patient about past prime ministers, dates of wars, and events that affect everyone.
Supported by the Netherlands Digestive Diseases Foundation (grant WS 94-24)
Received August 4, 1997; accepted February 25, 1998.
Address reprint requests to: Prof. Dr. S.W. Schalm, Dept. of Hepatogastroenterology & Internal Medicine II, Erasmus University Hospital Rotterdam, P.O. Box 2040, 3000 CA Rotterdam, The Netherlands. Fax: 31-10-436-5916.
Copyright © 1998 by the American Association for the Study of Liver Diseases